

 |  |
TRANSMYOCARDIAL REVASCULARIZATION
Transmyocardial revascularization (TMR), a new approach to the treatment of coronary artery disease, promises to offer an alternative to patients who do not respond to currently available forms of therapy, such as balloon angioplasty and coronary artery bypass grafting (CABG).
TMR involves use of a computer-controlled carbon dioxide laser to create new conduits for blood flow by boring small channels from the outside to the inside of the heart, specifically, the left ventricular cavity. These channels induce a natural process of healing called angiogenesis—that is, the growth of new blood vessels, which increase blood flow to feed oxygen-starved areas in the heart muscle.
Patients treated by TMR experience angina relief within weeks of sole therapy (TMR alone), or immediately when the technique is used in combination with CABG.
TMR has been studied extensively in experimental and clinical settings. The original investigational studies were conducted in the early 1970s. In recent years, nationally reported clinical studies indicate a lasting response at three years. When TMR is used in combination with CABG, three-year mortality rates are significantly reduced from about 12% to 4%.
Since TMR is performed on the beating heart without the use of cardiopulmonary bypass (CPB) via the heart-lung machine, this novel method of increasing blood flow to the heart may also be considered minimally invasive when used as sole therapy.
The adverse side effects associated with use of the heart-lung machine—which, during conventional CABG, takes over the stopped heart's work—are avoided. Patients do not experience the inflammatory response caused by CPB, which disrupts the body's physiologic balance.
TMR probably won't replace angioplasty or CABG surgery as the most common methods of treating coronary artery disease. These therapies have been proven over time to be safe, effective ways to restore blood flow to the heart muscle.
At present, the best candidates for TMR include patients who are high-risk candidates for a second bypass or angioplasty; patients whose blockages are too diffuse to be treated with bypass alone; and patients with heart transplants who develop atherosclerosis on the graft.
The Operation Itself
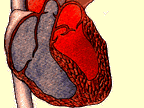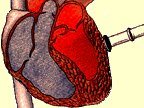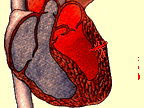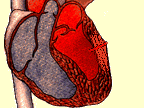 To perform TMR, the surgeon makes a limited incision on the left side of the chest and inserts a laser into the chest cavity. With
the laser, the surgeon shoots holes through the heart's left
ventricle in between heartbeats; the laser is fired when the
chamber is full of blood so the blood can protect the inside of the
heart.
To perform TMR, the surgeon makes a limited incision on the left side of the chest and inserts a laser into the chest cavity. With
the laser, the surgeon shoots holes through the heart's left
ventricle in between heartbeats; the laser is fired when the
chamber is full of blood so the blood can protect the inside of the
heart.
The characteristics of laser energy make it an ideal tool to use. The channels can be made with little damage to surrounding tissue, and they can be made quickly.
From 15 to 30 channels, each a millimeter in diameter, are opened. Then the surgeon presses a finger on the holes on the outside of the heart. This seals the outer openings but lets the inner channels stay open to stimulate the growth of new blood vessels.
The operation takes about two hours to complete. The average hospital stay following the procedure ranges from two to seven days, depending on whether TMR is used as sole therapy (about seven days) or in combination with different methods of CABG surgery (about two to five days).
TMR has received approval from the Food and Drug Administration for use in patients with severe angina who have no other treatment options.