

 |  |
OBESITY SURGERY PROGRAM RE-ESTABLISHED
![]() We are pleased to announce the re-establishment of our
bariatric surgery program for the treatment of morbid obesity.
The new program is directed by Collin E.M. Brathwaite, MD, associate professor of surgery and
chief of trauma/surgical critical care. An active general
surgeon, Dr. Brathwaite has considerable experience in nutrition
and currently chairs University Hospital's nutrition
committee.
We are pleased to announce the re-establishment of our
bariatric surgery program for the treatment of morbid obesity.
The new program is directed by Collin E.M. Brathwaite, MD, associate professor of surgery and
chief of trauma/surgical critical care. An active general
surgeon, Dr. Brathwaite has considerable experience in nutrition
and currently chairs University Hospital's nutrition
committee.
John S. Brebbia, MD, assistant professor of surgery, and Louis T. Merriam, MD, assistant professor of surgery, are also involved in the program. They both have a strong interest in nutrition and obesity surgery. In addition, nurse practitioner Barbara A. Smith, RN, MS, coordinates the program, including the patient support group.
Morbid obesity is that state where body weight exceeds ideal body weight by 100 pounds or more. Obesity of this degree is truly morbid since individuals with it face increased complications from their obesity or may be expected to die earlier than predicted on the basis of life-expectancy tables.
Recognizing that a multidisciplinary approach to the treatment of obesity is necessary, a special support group facilitated by the program's nurse practitioner supplements the surgical therapy. This group provides patients with psychological support to help ensure successful outcomes. It provides information and an opportunity to network with other patients considering or having had the surgery. The group meets on the first Tuesday of every month, from 5:15 PM to 6:30 PM, at the Baldwin Center at 37 Research Way in East Setauket. The group is open to the public. Individuals interested in attending must call 631-444-1045 to confirm their attendance: please leave voice message, plus name and phone number.
To contribute to efforts to further advance obesity surgery, the program is enrolled in the International Bariatric Surgery Registry (formerly known as the National Bariatric Surgery Registry). One of its goals is to enable surgeons to evaluate and improve their expertise in obesity surgery, and benefit from the combined experience of all participants.
Although our new obesity surgery program was just initiated in the summer, increasing numbers of patients are now seeking surgical therapy at University Hospital for critical weight management.
National Health Problem
Obesity is a national health problem of significant proportion. It is estimated that approximately 97 million adults in the United States are overweight or obese. The figures would be even higher if we considered overweight children.
The importance of this national health problem has been underscored by National Institutes of Health (NIH) consensus conferences. These conferences looked at two issues in the management of obesity: the role of surgery in the treatment of obesity and the role of conventional treatments, such as dieting, in the management of the overweight.
The reason why obesity is a health problem relates to the illnesses associated with, or caused by, obesity. Among these illnesses are diabetes, heart disease, high blood pressure, gallbladder disease, and cancer. This list is by no means complete, but does include some of the major medical problems that are associated with obesity. Although they are not caused exclusively by being overweight, they may be exacerbated by it, or they may be accelerated in their development.
The estimated cost to the American health care system for these problems is $70 billion per year. Thus, the impact of obesity becomes clearer, not only in terms of health and well-being, but also in economic terms.
The causes of obesity are not fully known or understood at the present time. Obesity is most likely a multi-causal problem, with contributions from several areas. There is certainly a genetic factor, since we know that obesity is frequently familial.
Certain endocrine diseases may also be associated with obesity. In our program, patients are screened for them as part of their work-up.
Extensive research is ongoing to discover the underlying cause of obesity beyond what is already known. Much of this research is looking at what controls satiety—the sensation of being "full" or satisfied. Some chemicals naturally produced by the body are among the prime candidates in these investigations.
Treatments for Obesity
The treatment of obesity is, like the cause, multi-modal. The major forms of treatment include dieting and behavioral modification. The greatest success in non-operative therapy is achieved by combination therapy which combines elements of behavior therapy (e.g., reinforcement, changes in attitudes about foods and eating), dieting, and exercise.
Through these means, patients decrease their intake of calories and increase the rate at which calories are used. Perhaps the most significant finding of the 1991 NIH Conference on Non-Operative Treatment of Obesity was the general lack of success of dieting alone. In fact, the use of dieting with its yo-yoing weight loss followed by weight regain may in fact be more harmful to the body than a small amount of obesity.
Commercial programs take advantage of the fact that, for the overweight individual, there very often is an initial gratifying weight loss by adherence to any single program. However, there tends to be a plateau in this rapid weight loss during which time many individuals drop out of the programs because they do not achieve the continuous ongoing weight loss that they find desirable.
Once commercial dieting programs have been abandoned, the weight that was initially lost then reaccumulates or sometimes accumulates to a degree that is even greater than the weight at the start of the program. This again leads to the yo-yoing up- and-down weight that has harmful effects on the body because of the frequent alterations in normal body maintenance, or homeostasis.
Thus, exercise must be introduced and maintained on a regular basis, and unhealthy foods or eating habits must for the most part be given up and totally abandoned. It is probably the inability to incorporate these necessary changes into one's life and lifestyle that prevent the usual means for the management of obesity from being as successful as they might otherwise be.
Surgery for Obesity
Surgery has been a treatment option since the early 1950s. Because surgical intervention is so invasive and, in a sense, radical, it is only indicated in selected patients. Obesity has degrees, and the patients who are candidates for surgery are those who are classified as morbidly obese.
The most effective procedures for weight loss utilize the principle of gastric restriction. If the stomach pouch is made smaller, this reduction will limit the amount an individual can eat and weight loss will result. The operations used include gastric banding, vertical banded gastroplasty, and Roux-en-Y gastric bypass (popularly known just as gastric bypass).
Our bariatric surgeons perform both vertical banded gastroplasty and gastric bypass—the two operations most commonly used today for treating obesity, both of which have been endorsed by medical experts assembled by the NIH. These experts concluded that surgery for obesity, with its high rate of success, is an option that should be considered after non-surgical weight-control measures have failed.
The following five criteria must usually be met before a patient can be accepted for weight loss surgery at Stony Brook: 1. You must be at least 100 pounds overweight with a body mass index greater than 40. 2. You must have at least one associated medical problem (such as high blood pressure or diabetes) or a body mass index greater than 50 without associated medical problems. 3. You must be a non-smoker. Smoking disqualifies patients from surgery, because it not only interferes with wound healing and causes respiratory complications, but counteracts all the medical benefits of weight loss. 4. You must have a sincere motivation to lose weight, including a willingness to make necessary changes in habits, to cooperate fully with instructions, and to keep appointments for follow-up visits. 5. You must be between 15 and 60 years of age, though this
requirement may vary in individual cases. |
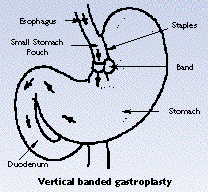
![]() Vertical banded gastroplasty creates a small upper pouch in
the stomach and then uses a vertical band of synthetic material
to restrict the opening between this upper pouch and the lower
stomach. Food then leaves the stomach in the normal fashion after
passing out of the upper pouch. Weight losses of 50% to 60% of
excess weight can be expected after this surgery.
Vertical banded gastroplasty creates a small upper pouch in
the stomach and then uses a vertical band of synthetic material
to restrict the opening between this upper pouch and the lower
stomach. Food then leaves the stomach in the normal fashion after
passing out of the upper pouch. Weight losses of 50% to 60% of
excess weight can be expected after this surgery.
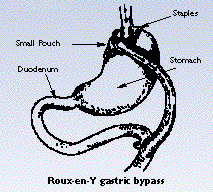
![]() Gastric bypass also creates a small upper pouch in the stomach
(about 1-2 ounces in size), but this pouch is completely
separated from the lower stomach by multiple rows of surgical
staples. To allow drainage from the stomach, this small pouch is
connected to the small intestine, a portion of which is
bypassed.
Gastric bypass also creates a small upper pouch in the stomach
(about 1-2 ounces in size), but this pouch is completely
separated from the lower stomach by multiple rows of surgical
staples. To allow drainage from the stomach, this small pouch is
connected to the small intestine, a portion of which is
bypassed.
The extra step of draining food from the upper pouch directly into the small intestine gives this operation an extra mechanism for weight loss because not all of the foods are as effectively absorbed (malabsorption). The weight loss with this procedure is considered successful when the mean excess weight lost is between 48% and 74%.
Both of these operations do require that patients change their eating habits. Because of the small size of the stomach pouches which are created surgically, large meals cannot be tolerated. Eating too much may result in regurgitation or vomiting.
In this fashion, behavior modification is enforced upon the patient. Patients are also advised to exercise to enhance their weight loss. For some patients this is a new experience since their preceding obesity may have made exercise impossible.
Dr. Brathwaite comments: "It is important to emphasize that surgery is not for everybody. Patients should come to the decision for surgery on their own and not be forced into it, since surgical therapy does require a number of changes in their lifestyle to be most effective. Support by the patient's family is crucial."
"However," he adds, "once patients do undergo the surgery, their future may be significantly changed, not only with respect to their health but also because of improved body image and psychosocial well-being."
Perhaps the most important things to recognize about obesity are the enormity of the problem and its associated risks. Whatever method of weight management is used is not as important as the pressing fact that obesity needs to be controlled.
For more information about the obesity surgery program, please call 631-444-1045.
| Back to Departmental News | Return to Home Page |