

 |  |
PERFORMING ENDOVASCULAR THORACIC AORTIC STENT GRAFTING: A Minimally Invasive Option for Repair of Aortic Aneurysms
![]() Thoracic aortic aneurysm (TAA) — a bulge in the major artery from the heart — is a life-threatening condition that potentially may cause death as a result of rupture or dissection (tearing) and subsequent internal bleeding. The natural history of TAA is incompletely understood, but its prevalence is increasing as the population ages.
Thoracic aortic aneurysm (TAA) — a bulge in the major artery from the heart — is a life-threatening condition that potentially may cause death as a result of rupture or dissection (tearing) and subsequent internal bleeding. The natural history of TAA is incompletely understood, but its prevalence is increasing as the population ages.
In fact, the incidence of TAA has increased more than three-fold in the past 40 years, partly because it is being identified more often than in the past by computed tomography (CT) of the chest, which is now more widely used to screen for other medical conditions. Most non-leaking TAAs are detected by tests such as chest x-ray or CT scan done for other reasons.
TAAs currently affect an estimated 21,000 individuals each year in the United States. However, they are generally believed to be significantly under-diagnosed because most people who have them experience no symptoms. Usually, no symptoms occur until the aneurysm begins to leak or expand.
Management of thoracic aortic disease can be complicated by the high morbidity (incidence of disease or medical conditions) associated with both medical and surgical treatment. Given the complexity of performing open surgical repair of the thoracic aorta and its associated morbidities such as heart attack, stroke, paralysis, kidney damage, and prolonged ventilator support, new approaches to thoracic aneurysm repair are being investigated.
Our cardiovascular specialists — cardiothoracic and vascular surgeons working together — perform the newly developed minimally invasive endovascular stent grafting repair of TAAs. The entire operation is done within the aorta itself, via its branches in the groin, using the endovascular approach (endo-, within + vascular, vessel) with the aid of special technology and instrumentation.

Because endovascular surgery involves a smaller incision, compared with that used in conventional operations, and also avoids the need for extracorporeal perfusion (use of heart-lung machine), it causes less disruption of the patient's physiology, or vital processes. Consequently, the hospital stay is usually much shorter and the patient's recovery much faster. Smaller scars are another major benefit.
Given that minimally invasive methods have been sought for decades, endovascular surgery — originally developed in the mid-1980s — is now a rapidly growing field of therapy. It may be used independently or in combination with conventional operations for treating cardiovascular disease.
At present, nearly every vascular bed in the body can be approached intraluminally (from within the vessels).
With the recent advent of the endograft, or "internal bypass" graft, the minimally invasive techniques of endovascular surgery can now be applied to treat aneurysmal as well as occlusive atherosclerotic disease-that is, to correct circulation problems in damaged or blocked arteries without having to resort to open surgery. TAA is one such problem.
Traditional operative management of thoracic aortic aneurysms involves extensive surgery requiring a large incision in the chest to place a synthetic graft to repair the diseased artery. This method can result in long hospital stays and painful recoveries. Today, we are seeking less invasive alternatives to this major open surgical approach. The revolutionary thoracic endoprosthesis means we now have a minimally invasive option for safely and effectively managing patients with aneurysms of the descending thoracic aorta.
About the Stent and the Operation
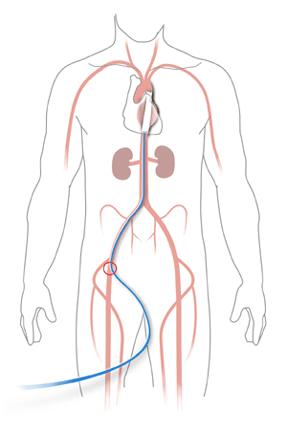
![]() The stent device we currently use in the endovascular repair of TAAs is a flexible tube that resembles a child's finger-trap toy. It is composed of an expanded polytetrafluoroethylene (ePTFE; similar to Gore-Tex fabric) graft with an outer self-expanding nitinol (nickel-titanium alloy) support structure to combine both device flexibility and material durability. It comes in a range of lengths and diameters.
The stent device we currently use in the endovascular repair of TAAs is a flexible tube that resembles a child's finger-trap toy. It is composed of an expanded polytetrafluoroethylene (ePTFE; similar to Gore-Tex fabric) graft with an outer self-expanding nitinol (nickel-titanium alloy) support structure to combine both device flexibility and material durability. It comes in a range of lengths and diameters.
The Food and Drug Administration, which approved the stent in March 2005 for descending TAAs, requires that surgeons have special training on how to use it. This stent, manufactured by W. L. Gore & Associates, is the first of its kind to gain FDA approval for use in TAA repair.
To implant the stent, our surgeons make a 2- to 4-inch incision in the patient's upper groin or abdomen and guide a catheter (thin flexible tube) with the compressed stent through an artery and into the diseased part of the aorta. When the catheter is withdrawn, the flexible stent springs open and expands to the width of the aorta, creating a new aortic lining and sealing off blood flow into the aneurysm "bubble."
Without blood to feed it, the repaired TAA typically shrinks over time.
Precise placement is crucial: Once the stent is expanded, it cannot be readjusted. Our surgeons test on computer models before surgery to see what stent length and diameter will work best. In the operating room they guide the stent to the proper position by real-time x-ray images viewed on a monitor.
In clinical trials, use of the endovascular stent had fewer deaths than traditional surgical treatments, less blood loss, a shorter hospital stay, and quicker recovery. Unlike open surgery, the stent can be implanted under local anesthesia.
Endovascular thoracic aortic stent grafting is also an option for elderly patients and others who would be unable to withstand the traditional surgery, which involves making a 12- to 14-inch-long opening in the chest and removing the diseased part of the aorta while the patient is kept alive on a heart-lung machine.
Since the stent has been used in trials only since 1999, it is unclear how long it will actually last. However, the device has held up so far in patients who have received it in the past several years.
Our Commitment to Excellence
Traditional surgical repair of TAAs carries significant risks even in otherwise healthy individuals. Unfortunately, thoracic aortic disease is most prevalent in elderly patients with multiple comorbidities (coexisting medical conditions), making them poor surgical candidates.
This complex situation poses a considerable challenge for physicians caring for patients with progressing or acute TAAs since the surgical treatment may pose as much or more risk to their health than does the disease itself.
As a result of the morbidity associated with traditional surgical repair of TAAs, there is significant potential for the use of new technological advances, such as endovascular stent grafting, allowing for aneurysm repair with minimal invasiveness and decreased operative risk.
Thoracic endografting now provides the only alternative for many high-risk patients with TAAs who are denied conventional surgery because of known morbidity and mortality.
At Stony Brook University Hospital, as a further demonstration of our commitment to excellence in patient care, we currently perform endovascular thoracic aortic stent grafting, and plan to use it in the future, as well, for the treatment of aortic transections and complicated dissections.

| Thoracic Aortic Aneurysm in Profile |
Location: TAA occurs in the ascending aorta (25% of the time), the aortic arch (25% of the time), or the descending thoracic aorta (50% of the time). Note that aneurysms can develop anywhere along the aorta: 75% develop in the abdominal aorta that runs through the belly, and the rest develop in the thoracic aorta in the chest.
Causes: The most common cause of TAA is atherosclerosis (hardening of the arteries). Other causes and/or risk factors include hypertension (high blood pressure); inherited connective tissue disorders, such as Marfan syndrome and Ehlers-Danlos syndrome; trauma, such as falls or motor vechicle accidents; smoking; previous dissection (tearing) of the aorta; and, rarely, infection that weakens a section of the aorta wall.
Incidence: TAA is diagnosed at a rate of 10.4 in 100,000 people per year, though under-diagnosis due to absence of symptoms is common. Of note, the incidence of TAA has increased more than three-fold in the past 40 years, because of the increasing elderly population, as well as the increased use of CT scanning for other conditions in the chest.
Mortality/Morbidity: The cumulative risk of TAA rupture is related to aneurysm diameter. In a recent series of 133 patients with TAA, risk of rupture at five years was 0% for diameter less than 4 cm (1½ inches), 16% for diameter 4-5.9 cm (1½ to 2¼ inches), and 31% for aneurysms greater than 6 cm (2½ inches) in diameter. Overall survival for thoracic aortic aneurysms has improved significantly in the past 15 years.
Race: TAA is most common among whites.
Sex: TAA affects both men and women at the same rate. Women are significantly older at their initial diagnosis than men, and rupture occurs more frequently in women.
Age: The average age of patients at diagnosis of TAA is 60-70 years, while the incidence of TAA increases dramatically with age.
Symptoms: Only 25% of individuals with TAA have symptoms, which result from the pressure of the enlarging aorta against nearby structures and thus depend on the aneurysm's location. Typical symptoms are pain (usually high in the back), coughing, and wheezing. Rarely, a person coughs up blood. Difficulty in swallowing or hoarseness may occur.
Ruptured TAA causes excruciating pain that usually begins high in the back. This pain may radiate down the back and into the abdomen as the rupture progresses. The pain may also be felt in the chest and arms, as it is during a heart attack. Emergency surgery is needed for survival.
Treatment: For TAA that is 6 cm (2½ inches) wide or larger, surgical repair using a synthetic bypass graft is usually performed. Surgery is also indicated for smaller aneurysms that are actively growing larger, or in patients with connective tissue disorders. Risk of death is about 5-15% during the repair (generally less when endovascular versus traditional open surgery), but is about 50% during an operation for a ruptured aneurysm. Untreated ruptured TAA is always fatal. Five-year survival for patients with unrepaired TAA greater than 6 cm is 20-25%.
